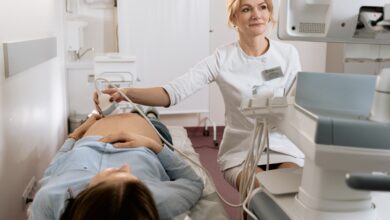
The first prenatal visit marks the start of the pregnancy follow-up which includes a total of seven visits. Complete, this first consultation aims to confirm the pregnancy, date it, monitor its progress, detect possible risky situations and put in addition a pregnancy calendar.
The first prenatal medical examination: when and why?
The first “official” prenatal visit must take place before the end of the 3rd month of pregnancy, i.e. 15 SA. This visit is the first of the 7 prenatal consultations provided for by the Public Health Code. It can be carried out by a medical gynecologist (who follows the pregnancy up to 6 months), a gynecologist-obstetrician (who follows the pregnancy and performs deliveries), a general practitioner (who can follow an uncomplicated pregnancy up to 8 months) or a midwife, in a practice in town, at the hospital, in a private clinic or by the maternal and child protection (PMI). It is up to the future mother to choose the practitioner and the place of follow-up of her pregnancy.
Often a first visit, earlier, can take place in order to confirm the pregnancy after the realization of the pregnancy test at home. The Haute Autorité de Santé also recommends that this first consultation be carried out a little earlier, before 10 WA, in order to be able to schedule the examinations on specific dates, in particular the first ultrasound, and to prescribe a prenatal check-up early and thus detect possible risky situations requiring monitoring or special precautions .
Questions asked by the gynecologist
The first prenatal visit is a little longer than the following ones because it has several objectives:
- make the diagnosis of pregnancy;
- date the pregnancy based on the date of the first day of the last menstrual period, and calculate the DPA, or expected date of delivery;
- ensure the smooth running of the early pregnancy;
- identify possible risky situations;
- set up pregnancy monitoring;
- give various advice to the future mother.
For this, the practitioner carries out a complete medical examination on:
- personal and family medical history (chronic pathology, hereditary disease);
- gynecological history: duration and regularity of cycles, miscarriage, ectopic pregnancy;
- obstetrical history: course of previous pregnancies and possible complications (gestational diabetes, IUGR, placenta previa, hypertension, pre-eclampsia, etc.), course of deliveries (vaginal route, instrumental extraction, cesarean section, obstructed delivery, premature delivery, etc.);
- the course of this early pregnancy and any ailments (nausea, vomiting, fatigue, constipation, etc.).
He then proceeds to a clinical examination comprising different aspects:
- a general examination with weight gain, blood pressure measurement, heart rate, examination of the lower limbs;
- a gynecological examination with a vaginal examination to determine the uterine volume and check whether it corresponds to the estimated age of pregnancy, a breast examination, a screening smear if the last is more than 3 years old;
- auscultation of the sounds of the heart of the fetus with ultrasound (possible from 12 SA), or a quick ultrasound check if the practitioner has a device in his office.
- bridge
- Allergies (overview)

- Achluophobia : all about the fear of the dark

- At what age can you do bodybuilding?

- Fatigue in the morning: causes and remedies

Compulsory exams
During this first prenatal visit, various examinations are prescribed for the mother-to-be. Some are required by law and therefore mandatory:
- if it is a first pregnancy, a blood group determination (A, B, O, complete rhesus and Kell phenotypes) if the future mother does not have a complete blood group card (two determinations);
- toxoplasmosis serology, unless the expectant mother’s immunity has already been tested and she can produce the test results;
- rubella serology, except in the case of written results less than one year old confirming immunity;
- screening for syphillis by blood test;
- glycosuria and albuminism (search for sugar and albumin in the urine);
- the search for irregular agglutinins (RAI) in order to detect a possible incompatibility between the mother and the fetus. In the event of a positive result, an identification and a titration of the antibodies will be carried out.
Other examinations are not compulsory but systematically prescribed and recommended:
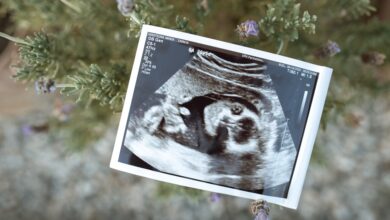
- the first ultrasound, to be performed between 11 SA and 13 SA + 6 days;
- combined screening for chromosomal abnormalities in the first trimester, including nuchal translucency measurement at the first ultrasound and a blood test for labeling of serum assays (PAPP-A and free b-hCG) between 8 and 14 WA;
- HIV 1 and 2 serology.
Depending on the interview and the clinical examination, the practitioner may be required to prescribe other examinations:
- a blood test to measure the beta-HCG in case of doubt about the pregnancy and its date;
- screening for anemia in the event of risk factors (vegetarian or vegan diet in particular);
- a cytobacteriological examination of the urine (ECBU) in the event of signs of urinary tract infection;
- a smear to screen for abnormalities of the cervix (cervical dysplasia) if the last one is 2 to 3 years old.
During this first visit, the practitioner can also prescribe vitamin B9 or folate supplementation to the future mother at the rate of 400 μg/day. This supplementation is recommended by the Haute Autorité de Santé up to 8 SA, in order to prevent neural tube defects.
If the mother-to-be suffers from a chronic pathology (arterial hypertension, diabetes), it may be necessary to adapt the current treatment.