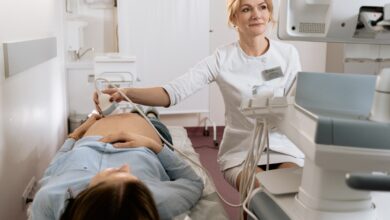
Constipation is one of the common pregnancy ailments. Due to various factors, transit tends to slow down in pregnant women. Lifestyle and dietary measures generally prevent constipation. In case of failure, the use of certain laxatives is possible.
Constipation, a well-known concern of pregnant women
Constipation concerns between 11 and 38% of pregnant women (1). It affects both future mothers usually prone to this transit problem and those who have never suffered from it before.
During pregnancy, various factors favor constipation:
- to promote the growth of the uterus, the strong secretion of progesterone leads to a relaxation of all the tissues, including the smooth muscles of the large intestine. Less toned, its motility is less effective and intestinal transit is slowed down;
- with the decrease in physical activity over the weeks, the intestine is mechanically less stressed and less well oxygenated;
- over the weeks, the uterus compresses the intestine more and more, the functioning of which, already slowed down under the effect of hormones, becomes even more sluggish;
- certain iron food supplements prescribed during pregnancy for the prevention or treatment of anemia can promote constipation, depending on the type of product.
Constipation is often more marked during the second part of pregnancy. It can last for two to three months after delivery. The transit then normally returns to its previous state.
What to eat against constipation during pregnancy?
Various lifestyle and dietary measures help prevent constipation during pregnancy. They are the same for the pregnant woman, as the rest of the population Namely:
- have a diet rich in fiber (fruits, especially cooked vegetables, wholemeal or semi-wholegrain cereals and bread, wheat, oat or rice bran, legumes, oilseeds), which facilitate intestinal transit. To avoid bloating, abdominal distension and gas, it is important to gradually increase your daily fiber intake. One can, for example, start by replacing white bread and refined cereals (pasta, rice) with their semi-complete version. If raw vegetables and fruits cause bloating, prefer their cooked version;
- hydrate sufficiently, with 1.5 to 2 liters of water. Ideally, choose it rich in magnesium, a mineral that promotes transit. To hydrate, also think of herbal teas, broths, diluted fruit juice;
- prunes are known to promote transit thanks to a substance called dihydroxyphenylisatin, which stimulates peristalsis (muscle contractions of the digestive system). To consume at the rate of 2 to 3 per day in dried form or in the form of juice;
- favor dairy products with active bifidus, a probiotic that helps regulate intestinal transit;
- flax seeds, rich in mucilages (fibers not absorbed by the intestine) can be added at the rate of a spoon, ground in a yogurt.
On the other hand, all foods and drinks that are difficult to digest or tend to cause gas should be limited: fried foods, dishes in sauce, pastries, carbonated drinks, etc. Some foods such as white rice, chocolate, bananas, cooked carrots are also known to slow transit (hence their recommended consumption in case of diarrhea).
- bridge
- Allergies (overview)
- Achluophobia : all about the fear of the dark
- At what age can you do bodybuilding?
- Fatigue in the morning: causes and remedies
Good everyday gestures
On a daily basis, various actions help prevent or treat constipation:
- maintain regular physical activity adapted to pregnancy (walking, swimming, gentle gymnastics). By exerting a kind of massage on the intestines through a mechanical effect, moving can indeed stimulate transit;
- when you get up, drink a large glass of cold water to wake up the transit;
- have a bowel movement as often as necessary and avoid holding back;
- in the saddle, adopt the most effective position for defecation: the knees raised above the hips, for example by placing a small step stool under the feet.
When should you consult?
If constipation persists despite hygiene and dietary measures, do not hesitate to talk to your doctor, gynecologist or midwife. It is important to find a good transit for its daily comfort but also to prevent hemorrhoids favored by constipation due to the effort of pushing, but also urinary tract infections.
In addition, in the event of bleeding during bowel movements, vomiting, abdominal pain and cessation of digestive gases, a rapid consultation is essential in order to rule out any risk of intestinal obstruction.
Finally, if the constipation appeared or worsened after the start of taking iron supplements, talk to your doctor about it in order, possibly, to change the supplementation to a more easily assimilated form.
Some laxatives can be prescribed during pregnancy while others should be avoided. The Reference Center for Teratogenic Agents in Pregnant Women (2) thus recalls that the following two types of laxatives are to be preferred during pregnancy:
- bulk laxatives: these are fibres, generally mucilages alone or in combination, derived from gum (guar), seeds (sterculia, ispaghul, psyllium) or bran. Not absorbed by the digestive tract, they increase the volume and hydration of the stools and thus promote transit;
- osmotic laxatives: based on polyethylene glycol (PEG) or sugars such as lactulose, lacticol or sorbitol, they act by increasing the volume of salts.
Occasional use of a lubricating laxative such as unassociated paraffin oil is possible but not recommended during pregnancy, as it may reduce the absorption of fat-soluble vitamins (A, D, E, K).
Stimulant laxatives based on anthracenics (extracts of various plants: aloe, anise, fucus, buckthorn, boldo, tamarind, cascara, senna), sodium docusate, bisacodyl or picosulfate are not recommended during pregnancy with the exception of senna, whose data concerning pregnant or breastfeeding women are numerous and reassuring.